by Dr. Demitri Adarmes
What is an epidural injection?
The epidural injection, or epidural steroid injection, refers to a technique that has been used since the 1950s to provide relief of pain from the spinal cord. This is an invasive procedure that is considered after conservative and medical interventions to relieve pain have failed.
While this technique has been used effectively to relieve pain, it can also be used to allow a comprehensive physical therapy and rehabilitation program. This technique has been shown to be as effective as other more invasive techniques (such as neurolytic blocks), and should be considered.
Epidural injections have been used in a wide variety of conditions, particularly those causing pain from inflammation and irritation of the spinal nerves. The relief of pain can last anywhere from a week to a whole year, depending on the specific circumstances. Patients who receive epidural injections may come back several times a year for the procedure.
How does an epidural steroid injection work?
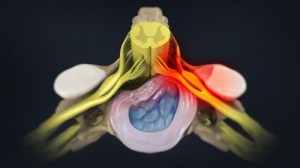
The epidural space, or the “extradural space”, refers to the anatomic space that lies outside the dura mater (the tough, fibrous material that encloses the spinal cord, the arachnoid matter, the subarachnoid space, the spinal fluid, etc.). This outermost chamber contains many important structures, such as the spinal nerve roots, venous plexuses, the lymphatic system, blood vessels and fatty tissues.
The epidural injection delivers steroids directly into the epidural space. The most commonly used steroids include dexamethasone, methylprednisone, and other corticosteroids. These powerful anti-inflammatory drugs provide relief by suppressing the inflammatory response. This, in turn, lessens the irritation and swelling of the nerve root, relieving the mechanical and chemical sources of pain.
What conditions can be treated with epidural steroid injections?
Epidural steroid injections have been used for conditions that cause nerve irritation. These include, among others, condition such as:
- Lumbar spinal stenosis
- Vertebral compression fractures
- Synovial cysts in the spine
- Herniation of intervertebral discs
- Lumbar Degenerative Disc Disease
Patients who have any of the following conditions are advised to avoid the procedure:
- Pregnancy (if the procedure is done under fluoroscopy/X-ray/CT guidance)
- Local or systemic infection
- Medical history of bleeding and clotting disorders
- Pain suspected to be secondary to a spinal tumor
- Uncontrolled medical problems (heart, liver, lung diseases)
- High does use of aspirin and other anti-platelet drugs
How is the epidural steroid injection procedure performed?
The procedure is typically done under a local anesthetic. This will allow the Workers Compensation pain management doctor to assess the success of the procedure intra-operatively. A mild sedative may be given to the patient.
Prior to the procedure, the procedure site will be scrubbed with a sterilizing solution, such as povidone-iodine, or chlorhexidine. Sterile linen will be draped around the area to provide a sterile operating feel.
Caudal Epidural Injection
The procedure begins when the Arizona workers compensation doctor inserts the needle into the injection site. There are different approaches to the epidural steroid injection: caudal, transforaminal and laminar. The injection is done under fluoroscopic (X-ray) guidance, although alternative guiding techniques using ultrasonography and computerized tomography (CT) scans have also been used.
With the caudal approach, the needle is inserted from the bottom-most (caudal) area near the sacrum (tailbone). This technique has been reported to give up to 75% of patients relief from low-back pain conditions.
The transforaminal approach injects the steroid into the opening of the spine (foramen) where the nerve root exits. There is a “root sleeve” that exists just outside the spinal canal; hence, the procedure is also known as a “root sleeve block”. This technique is preferred to the caudal approach because of the shorter operative times, and lower radiation exposure from fluoroscopy guidance.
The interlaminar approach injects the steroid from the back of the patient. This technique has also been shown to be effective in providing relief from pain.
Once the needle is in the proper place, the local anesthetic and/or the corticosteroid is injected. If the operation is successful, the patient will report an immediate relief of the pain. The surgeon may ask the patient to perform the range of motion that triggers the pain: if the pain is absent following the injection, then the patient is observed for 20 – 30 minutes before being sent out for recovery. The patient may be sent home the same day if no complications are noted.
What are the success rates?
Success rates are typically high for this procedure. Studies have shown relief of symptoms for more than 80% of those undergoing the procedure for lumbar disc herniation, while 75% of  patients undergoing the procedure for spinal stenosis report more than 50% reduction in pain over 1 year.
patients undergoing the procedure for spinal stenosis report more than 50% reduction in pain over 1 year.
As with any pain procedure, there are risks with epidural steroid injections. Patients may suffer from infection of the surgical site, intraoperative damage to muscles, nerves and tissues, or bleeding and hematoma formation may occur. It is advisable to discuss the procedure with an experienced surgeon prior to giving consent.






Leave A Comment